What is the prostate?
BPH stands for benign prostatic hyperplasia. Benign means “not cancer,” and hyperplasia means too much growth. The result is that the prostate becomes enlarged. BPH is not linked to cancer and does not raise your chances of getting prostate cancer–yet the symptoms for BPH and prostate cancer can be similar.
Symptoms
BPH symptoms usually start after the age of 50. They can include:
- Trouble starting a urine stream or making more than a dribble
- Passing urine often, especially at night
- Feeling that the bladder has not fully emptied
- A strong or sudden urge to pass urine
- Weak or slow urine stream
- Stopping and starting again several times while passing urine
- Pushing or straining to begin passing urine
At its worst, BPH can lead to:
- A weak bladder
- Backflow of urine causing bladder or kidney infections
- Complete block in the flow of urine
- Kidney failure
BPH affects most men as they get older. It can lead to urinary problems like those with prostatitis. By age 60, many men have signs of BPH. By age 70, almost all men have some prostate enlargement. The prostate starts out about the size of a walnut. By the time a man is 40, it may have grown slightly larger, to the size of an apricot. By age 60, it may be the size of a lemon.
As a normal part of aging, the prostate enlarges and can press against the bladder and the urethra. This can slow down or block urine flow. Some men might find it hard to start a urine stream, even though they feel the need to go. Once the urine stream has started, it may be hard to stop. Other men may feel like they need to pass urine all the time or are awakened during sleep with the sudden need to pass urine.
Early BPH symptoms take many years to turn into bothersome problems. These early symptoms are a cue to see your doctor.
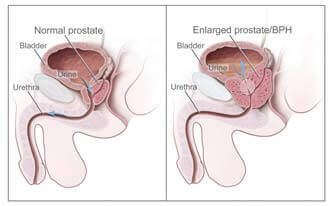
Urine flow of normal (left) and enlarged prostate (right). In diagram on the left, urine flows freely. On the right, urine flow is affected because of the prostate pressing on the bladder and urethra.
How can BPH be treated?
About half the men with BPH eventually have symptoms that are bothersome enough to need treatment. BPH cannot be cured, but drugs or surgery can often relieve its symptoms. BPH symptoms do not always grow worse.
There are three ways to manage BPH:
- Watchful waiting (regular follow-up with your doctor)
- Drug therapy
- Surgery
Talk with your doctor about the best choice for you. Your symptoms may change over time, so be sure to tell your doctor about any new changes.
Watchful waiting
Men with mild symptoms of BPH who do not find them bothersome often choose this approach.Watchful waiting means getting annual checkups. The checkups can include DREs and other tests (see “Types of Tests”). Treatment is started only if symptoms become too much of a problem.If you choose to live with symptoms, these simple steps can help:
- Limit drinking in the evening, especially drinks with alcohol or caffeine.
- Empty the bladder all the way when you pass urine.
- Use the restroom often. Don’t wait for long periods without passing urine.
Drug therapy
There are two main types of drugs used. One type relaxes muscles near the prostate while the other type shrinks the prostate gland. There is evidence that shows that taking both drugs together may work best to keep BPH symptoms from getting worse.
BPH surgery
The number of prostate surgeries has gone down over the years. But operations for BPH are still one of the most common surgeries for American men. Surgery is used when symptoms are severe or drug therapy has not worked well.
Types of surgeries include:
- TURP (transurethral resection of the prostate) is the most common surgery for BPH. It accounts for 90 percent of all BPH surgeries. The doctor passes an instrument through the urethra and trims away extra prostate tissue. A spinal block is used to numb the area. Tissue is sent to the laboratory to check for prostate cancer. TURP generally avoids the two main dangers linked to other prostate surgeries, which are Incontinence (not being able to hold in urine) and Impotence (not being able to have an erection).The recovery period for TURP is much shorter as well.
- TUIP (transurethral incision of the prostate) is similar to TURP. It is used on slightly enlarged prostate glands. The surgeon places one or two small cuts in the prostate. This relieves pressure without trimming away tissue. It has a low risk of side effects. Like TURP, this treatment helps with urine flow by widening the urethra.
- TUNA (transurethral needle ablation) burns away excess prostate tissue using radio waves. It helps with urine flow, relieves symptoms, and may have fewer side effects than TURP. Most men need a catheter to drain urine for a period of time after the procedure.
- TUMT (transurethral microwave thermotherapy) uses microwaves sent through a catheter to destroy excess prostate tissue. This can be an option for men who should not have major surgery because they have other medical problems.
- TUVP (transurethral electroevaporation of the prostate) uses electrical current to vaporize prostate tissue.
- Open prostatectomy means the surgeon removes the prostate through a cut in the lower abdomen. This is done only in very rare cases when obstruction is severe, the prostate is very large, or other procedures can’t be done. General or spinal anesthesia is used and a catheter remains for 3 to 7 days after the surgery. This surgery carries a higher risk of complications than medical treatment. Tissue is sent to the laboratory to check for prostate cancer.








