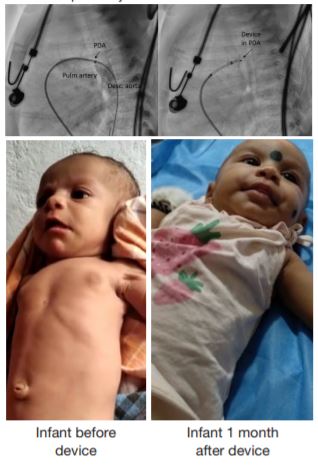
Device Closure Of Patent Ductus Arteriosus In A 2200 Gm Infant
A 2-month-old infant born at 37 weeks gestation with a birth weight of 2.3 kg presented with a history of shortness of breath during feeds, excessive sweating and poor weight gain since birth. Patent ductus arteriosus (PDA) was diagnosed in the nursery, treated with Ibuprofen and discharged on 8th day of life. The exam showed a thin built 2.2 kg infant in heart failure. Imaging revealed a hemodynamically significant 3 mm PDA (Type A) with the left to right shunt. We chose to do a transcatheter closure of this PDA instead of surgical ligation which has been the procedure of choice for small infants weighing < 5 kg.
The procedure was done under conscious sedation via right femoral venous access. Arterial access was avoided to minimize vascular complications, common in small infants. PDA was crossed from the main pulmonary artery and a wire was placed in descending aorta. A 4F TorqVue LP catheter (Abbott Medical, MN) was passed over this wire, minimal contrast was injected for a roadmap. An ADOII AS (Amplatzer) size 4/5 mm was deployed across the PDA using fluoroscopic and transthoracic echo guidance. After checking the optimal position and absence of residual shunt, the device was released. The procedure was uncomplicated and an infant was discharged the following day. Heart failure medications were stopped.
Infant continued to do well and gained 700 gm within a week. At her last follow up, one month after the procedure, the child weighed 3.7 kg and her heart failure symptoms resolved completely
Patent Ductus Arteriosus
Patent ductus arteriosus (PDA), a persistent communication between the descending thoracic aorta and the pulmonary artery is one of the most common congenital heart defects. It results in a significant left-to-right shunt contributing to pulmonary congestion, heart failure and poor growth in children and if left untreated, can result in pulmonary vascular obstructive disease and Eisenmenger’s syndrome. In the newborn, it
contributes to respiratory distress syndrome, prolonged assisted ventilation, bronchopulmonary dysplasia, increased risk of necrotizing enterocolitis, renal insufficiency, intraventricular haemorrhage, and increased overall morbidity and mortality, particularly in premature neonates.
Management of PDA in the premature infants includes medical therapy, failure of which necessitates surgical ligation. Transcatheter PDA closure, initially established as the procedure of choice for infants >5 kg, is can now be used in neonates and smaller infants due to advances in device design and interventional techniques. This avoids surgical ligation which is associated with significant perioperative complications. Percutaneous device closure, on the other hand, is minimally invasive, has lower complication rates and shorter hospital stay.